| Baptist Inpatient Radiology at Mississippi Baptist Medical Center | |
|---|---|
| Phone: | 601-968-1722 |
| Fax: | 601-968-1748 |
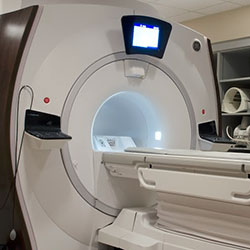
Magnetic resonance imaging (MRI) is a noninvasive, usually painless medical test that helps physicians diagnose and treat medical conditions.
MR imaging uses a powerful magnetic field, radio waves and a computer to produce detailed pictures of organs, soft tissues, bone and virtually all other internal body structures. The images can then be examined on a computer monitor or printed. MRI does not use ionizing radiation (x-rays).
Detailed MR images allow physicians to better evaluate parts of the body and certain diseases that may not be assessed adequately with other imaging methods such as x-ray,ultrasound or computed tomography (also called CT or CAT scanning).
For more information visit www.radiologyinfo.org.
Bring your insurance cards. Your insurance may require you to make a co-payment.
If you have had previous MRI studies from another facility not covered by the Radiological Group, please try to bring us a copy of that study and/or study report, if possible.
You should wear clothing without zippers and metal snaps. Jewelry such as watches, earrings, bracelets, and necklaces have to be taken off before entering MRI scanner area.
Follow the directions given for the location you are visiting found on our location pages. Upon arriving, check in with the receptionist who may have information for you to fill out. These forms are also available online. If you wish to fill them out ahead of time click here.
Once all your information has been obtained and processed, your technologist is notified of your arrival.
Your MRI technologist will talk with you before the exam, answering any questions you may have and asking you a series of screening questions to make sure you are a candidate for an MRI. People with electronic and metallic internal objects such as cardiac pace-makers, aneurysm clips, medication pumps, cochlear implants, etc. most often will not be able to have an MRI due to possible interactions between the magnetic and these devices. Click here for more information.
Some patients who have MRI in an enclosed scanner may feel confined, closed-in, and frightened. Perhaps one in twenty will require a sedative to remain calm. We have an “open” MRI at our Madison facility which is specifically designed to help those with claustrophobia. We will also permit a relative or friend to be present in the MR system room, which also has a calming effect. If patients are properly prepared and know what to expect, it is almost always possible to complete the examination.
You will placed on the MRI table. Once you are comfortable the table moves into the magnet. The MR machine makes a series of high volume sounds as it is acquiring images. You will be given ear plugs to help with the noise level. Alternatively, you can have earphones and listen to your favorite music during the study.
Depending on the type of MRI you are having, you may need intravenous or “IV” contrast which will be given through an IV line. The radiologist or technologist may ask if you have allergies of any kind such as hay fever, hives, allergic asthma, or to food or drugs. However, the contrast material used for an MRI exam, called gadolinium, does not contain iodine and is less likely to cause an allergic reaction.
One of the keys to an optimal study is to try to keep the body part being imaged as still as possible. For example, your knee for a MRI of the knee or your head for an MRI of the brain.
Study times vary based on the body part being imaged. Times may range from 20 to 45 minutes depending on the type of study. Times may be longer if your having multiple body parts imaged.
Any IV line will be removed. If you are undressed for the exam, you are taken back to the dressing room to put your clothes back on. Once the radiologist reviews your study and it is determined that no additional images or studies are needed, you will check out at the front desk. Depending on the order from your doctor, you will either stay while the report is given to your doctor or you will be free to leave and your doctor will discuss the study and results with you at a later time. All patients having an MRI are given a CD copy of their MRI study before leaving the facility.
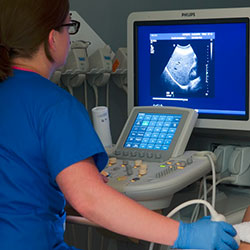
Ultrasound imaging, also called ultrasound scanning or sonography, involves exposing part of the body to high-frequency sound waves to produce pictures of the inside of the body. Ultrasound exams do not use ionizing radiation (x-ray). Because ultrasound images are captured in real-time, they can show the structure and movement of the body’s internal organs, as well as blood flowing through blood vessels.
Ultrasound imaging is usually a painless medical test that helps physicians diagnose and treat medical conditions.
Conventional ultrasound displays the images in thin, flat sections of the body. Advancements in ultrasound technology include three-dimensional (3-D) ultrasound that formats the sound wave data into 3-D images. Four-dimensional (4-D) ultrasound is 3-D ultrasound in motion.
A Doppler ultrasound study may be part of an ultrasound examination.
Doppler ultrasound is a special ultrasound technique that evaluates blood as it flows through a blood vessel, including the body’s major arteries and veins in the abdomen, arms, legs and neck.
For more information on ultrasound please visit radiologyinfo.org.
Abdomen or gallbladder ultrasound: Do not eat or drink after midnight (NPO), including no smoking or gum chewing. You may brush your teeth.
Pelvic Ultrasound: Do not go to the bathroom 2 hours before the exam. During the first hour before the exam, you need to drink one 8 ounce glass of clear liquid every 15 minutes. It can be any clear liquid (Kool-aid, coffee, coke, etc. Examples of nonclear liquids are milk or juice.) Stop drinking 1 hour before exam.
For example: If appointment time is 2:00 PM, do not go to the bathroom after 12:00 noon. Starting at 12 noon until 1:00 PM, drink one glass of water every 15 minutes. Stop drinking the water at 1:00 PM. Patient may come in early to complete paperwork, 15 minutes is usually enough time to complete the paperwork.
Abdomen and pelvic ultrasound: Do not eat after midnight. NO FOOD. Drink one 8 ounce glass of water every 15 minutes beginning 2 hours before appointment time. This will be a total of four 8 ounce glasses (32 ounces). Stop drinking one hour before your appointment time.
Renal ultrasound: You may eat or drink with no restrictions. Do not go to the bathroom one hour before the examination. You do not need to force fluids, just have a normally full bladder until the examination is completed.
All other types of ultrasounds: There are no preparations for other ultrasound examinations except for biopsies.
You need to bring your insurance card and driver’s license. You will not need a driver. You will not receive any medication.
You will be asked to remove most of your clothing and instructed to put on a gown. Sonograms require a gel be applied to your skin. This is so our transducer will glide across your skin and to insure there is contact between your skin and the transducer.
Follow the directions given for the location you are visiting found on our location pages. Upon arriving, check in with the receptionist who may have information for you to fill out. These forms are also available online. If you wish to fill them out ahead of time click here.
Once all your information has been obtained and processed, your technologist is notified of your arrival.
You will lie on an examination table. A warm gel will be applied to your skin, then a small instrument called a transducer will be moved across your skin. The transducer sends sound waves into your body. These high frequency sound waves are reflected back to the transducer. This information is processed by the ultrasound machine in real time producing sonographic images of the inside of your body. You cannot hear the sounds and the study is generally painless.
If you are female and are having a pelvic ultrasound, an endovaginal scan may be performed. This may be a little uncomfortable but should not be painful.
The most important thing is for you to follow the instructions for the preparation before the sonogram. During the study, you may be asked to take in a deep breath which helps move your internal organs away from bone and gas (as is in your stomach and colon). These structures can limit sonographic visualization.
Most examinations take 15-30 minutes.
If you are undressed for the exam, you are taken back to the dressing room to put your clothes back on. Once the radiologist reviews your study and it is determined that no additional images or studies are needed, you will check out at the front desk. Depending on the order from your doctor, you will either stay while the report is given to your doctor or you will be free to leave and your doctor will discuss the study and results with you at a later time.
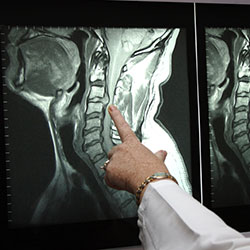
The chest x-ray is the most commonly performed diagnostic x-ray examination. A chest x-ray produces images of the heart, lungs, airways, blood vessels and the bones of the spine and chest.
An x-ray (radiograph) is a noninvasive medical test that helps physicians diagnose and treat medical conditions. Imaging with x-rays involves exposing a part of the body to a small dose of ionizing radiation to produce pictures of the inside of the body. X-rays are the oldest and most frequently used form of medical imaging.
There are many other uses of XRay other than Chest. Please use this link to learn more:
http://www.radiologyinfo.org/en/sitemap/modal-alias.cfm?modal=xray
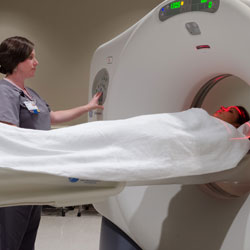
Computed Tomography (CT) System, also know as a “CAT Scan” is a medical diagnostic tool that allows the visualization of internal structures within the human body. This aids physicians in diagnosing disease, viewing internal abnormalities and assessing the extent of trauma damage.
During a typical CT procedure, the patient is placed on a table. The table then moves the patient through the gantry (a donut-shaped device), which houses an X-ray tube and detector array. For each image acquired, the X-ray tube rotates around the patient and the X-rays pass through the patient to the detector array, and thousands of X-ray measurements are acquired. The computer then processes this information and displays the corresponding images on a computer screen. This imaging technique avoids any superimposition of organs or tissues upon one another that might occur during other types of X-ray tomographic studies.
The CT exam creates images analogous to a single slice of bread from a whole loaf or a slice from an orange. Hence, the word ‘slice’ is often used to describe a view of patient anatomy.
The quality of an image depends on the nature of the X-ray source and detectors, the number and speed of the measurements made, the details of the reconstruction technique (algorithm), the machine characteristics, and the methods of data display and interpretation. The computer allows healthcare professionals to shade, rotate, correlate and measure anatomy in the image. This data can be manipulated to derive even more precise clinical information. While conventional X-ray can discern tissue density difference of five percent, CT can distinguish a density difference of 1 percent or less, aiding in diagnostic confidence.
For more information, visit RSNA’s radiologyinfo.org website.
If you are having a CT of your abdomen and/or pelvis, you might have to drink oral contrast material which is given to coat the intestines. This is usually given before the exam. Therefore, we ask that you have nothing to eat or drink after midnight on the night before your exam.
Depending on the type of CT you are having, you may need intravenous or “IV” contrast which will be given through an IV line immediately before the study. IV contrast is given to enhance the blood vessels that feed your organs. We ask that you do not eat a heavy meal before your exam as, occasionally, patients receiving IV contrast who have had a heavy meal may experience mild nausea. During the study, IV contrast may make you feel warm all over. This can last for about 1 minute and is normal.
Please let us know ahead of time if you have a history of kidney disease or renal failure. If this is the case, you may need a blood test to determine your kidney function if you are to receive IV contrast.
If you are having a CT that requires IV contrast and are taking a medication for diabetes known as Metformin (Glucophage, Glucovance, etc.), you will need to stop taking this medication during the two days following your exam. Also, your doctor may need to order labwork to check your renal function. Your doctor will be aware what to do in this event.
We recommend drinking plenty of fluids after your exam to flush both the IV and oral contrast from your system.
Bring your insurance cards. Your insurance may require you to make a co-payment.
If you have had previous CT studies from another facility not covered by the Radiological Group, please try to bring us a copy of that study and/or study report, if possible.
We recommend wearing comfortable clothes that do not contain any metal in the area we are going to be imaging. We have gowns for you to change into in cases where this is needed.
Follow the directions given for the location you are visiting found on our location pages. Upon arriving, check in with the receptionist who may have information for you to fill out. These forms are also available online. If you wish to fill them out ahead of time click here.
Once all your information has been obtained and processed, your technologist is notified of your arrival.
The technologist will take you to the CT suite and ask you a series of history questions that aid in the reading of your exam. If needed, you may be given a cup of oral contrast to drink. If IV contrast is needed, the technologist will start an IV line. Once everything is ready, the technologist will start your study. You may be given breathing instructions during your study if needed for your exam.
During a CT scan, the images are obtained in a matter of seconds. During the scan, you are asked to hold still and sometimes hold your breath for a few seconds. Following these instructions can improve the image quality of your study.
CT studies usually range from 5-10 minutes though may be longer if it is determined during your study that additional images are needed.
Any IV line will be removed. If you are undressed for the exam, you are taken back to the dressing room to put your clothes back on. Once the radiologist reviews your study and it is determined that no additional images or studies are needed, you will check out at the front desk. Depending on the order from your doctor, you will either stay while the report is given to your doctor or you will be free to leave and your doctor will discuss the study and results with you at a later time.

A video fluoroscopic swallowing exam (VFSE), also sometimes called a modified barium swallow exam (MBS), or swallow study, is a radiologic examination of swallowing function that uses a special movie-type x-ray called fluoroscopy. The patient is observed swallowing various types of substances that can be seen by fluoroscopy (usually liquid barium and/or foods coated with barium) in order to evaluate his or her ability to swallow safely and effectively. Patients are often observed swallowing various consistencies and textures, ranging from thin barium to barium-coated cookies. This exam is often performed with a speech-language pathologist present.
An x-ray (radiograph) is a noninvasive medical test that helps physicians diagnose and treat medical conditions. Imaging with x-rays involves exposing a part of the body to a small dose of ionizing radiation to produce pictures of the inside of the body. X-rays are the oldest and most frequently used form of medical imaging.
Fluoroscopy allows imaging of anatomical structures in real-time and allows the interpreting physician to observe structure and limited function.
A VFSE may be performed as an independent test to look at the motion of the throat during swallowing, or together with anesophagram, also called a barium swallow exam, which evaluates the structure and function of the esophagus to the level of the stomach.
The VFSE is used in patients of all ages with dysphagia, the technical term for difficulty swallowing. It is used primarily for evaluation of the swallowing function and any evidence of aspiration, which is liquid or food going into the airway (the trachea) instead of staying in the pharynx and esophagus.
In order to help a patient swallow more safely and efficiently, experts such as speech-language pathologists may suggest certain maneuvers, such as chin tuck or tilting or turning the head while swallowing. The VFSE can also be used to evaluate and observe how well such swallowing strategies work in a given patient.
The VFSE exam may be performed because of a known or suspected swallowing problem or because of the presence of conditions that are strongly associated with swallowing difficulty, such as:
You should inform your physician of any medications being taken and if there are any allergies, especially to iodinated contrast materials. Also inform your doctor about recent illnesses or other medical conditions.
Other than medications, you may be instructed to not eat or drink anything for several hours before your procedure.
You will also be asked to refrain from smoking or chewing gum prior to the exam.
You may be asked to remove some or all of your clothes and to wear a gown during the exam. You may also be asked to remove jewelry, removable dental appliances, eye glasses and any metal objects or clothing that might interfere with the x-ray images.
Women should always inform their physician and x-ray technologist if there is any possibility that they are pregnant. Many imaging tests are not performed during pregnancy so as not to expose the fetus to radiation. If an x-ray is necessary, precautions will be taken to minimize radiation exposure to the baby. See the Safety page for more information about pregnancy and x-rays.
Video fluoroscopic swallowing studies are also commonly performed on infants and children. Your doctor will give you detailed instructions to prepare your child for the examination. You may be asked to bring small amounts of the foods and liquids your child is able to eat and drink as well as things he or she has difficulty swallowing. You may also be asked to bring the things your child normally uses when eating or drinking, such as the bottles and nipples you use at home, sipper (“sippy”) cups, and/or eating utensils such as spoons.
The foods you bring to the exam will be mixed with a material called barium that will show up on the x-ray. You may want to explain to your child that the barium may change the way the food looks and tastes.
X-rays are a form of radiation like light or radio waves. X-rays pass through most objects, including the body. Once it is carefully aimed at the part of the body being examined, an x-ray machine produces a small burst of radiation that passes through the body, recording an image on photographic film or a special detector.
Fluoroscopy uses a continuous or pulsed x-ray beam to create a sequence of images that are projected onto a fluorescent screen, or television-like monitor. When used with a contrast material, which clearly defines the area being examined by making it appear dark (or by electronically reversing the image contrast to white), this special x-ray technique makes it possible for the physician to view joints or internal organs in motion. Still images or movies are also captured and stored electronically on a computer.
Until recently, x-ray images were maintained as hard film copy (much like a photographic negative). Today, most images are digital files that are stored electronically. These stored images are easily accessible and are frequently compared to current x-ray images for diagnosis and disease management.
The VFSE exam may also be recorded on a DVD or on another medium.
Your physician or speech-language pathologist will take your medical history, including complaints of difficulty swallowing.
A radiologist or radiologic technologist and a speech-language pathologist will guide you through the swallow exam.
You will be positioned upright on a chair or stool or be standing on a platform. If necessary, you may remain in a wheelchair.
You will be directed to eat and drink controlled amounts of foods and liquids in a variety of consistencies to which barium, acontrast material, has been added. The speech pathologist may try to help you swallow better by using different cups or utensils or changing your body position.
As you eat and drink, the x-ray camera will be moved near your throat. The speech-language pathologist and radiologist will watch you swallow in real-time through a fluoroscope, a device that projects radiographic images in a movie-like sequence onto a monitor. The images are usually captured digitally, so they can be reviewed later.
The imaging portion of this procedure is usually completed within 15 minutes.
You may find the taste and consistency of the barium unpleasant.
After the examination, you can resume your usual diet and take orally administered medications unless told otherwise by your doctor. You may also resume your normal activities.
For a day or two following your exam, your bowel movements may look white because of the barium. White bowel movements are normal. Sometimes the barium can cause temporary constipation, which is usually treated by an over-the-counter laxative.
Drinking increased quantities of fluids for several days following the test can also help. If you are unable to have a bowelmovement, or if your bowel habits undergo any significant changes following the exam, you should contact your physician.